Excess Mortality in Canada: Part 1
I thought it might be interesting to apply the excess mortality analysis that I've used for Ontario to Canada as a whole. The same trends appear, of course, but now with even more empirical grounding. For those who haven't read my earlier posts on this, the idea is to compare a ten-year baseline of excess mortality to three full years of Covid response policy, up to March of 2023. It's a simple approach: chart actual total annual deaths in each age category over ten years (March 2010 to March 2020); add a trend line to show expected deaths for the period in question (March 2020 to March 2023); calculate approximate excess deaths in 2020-2023 (i.e. amount above trend line); compare the results to official figures for 'Covid deaths' during the same period. As before, to make for a fair comparison, I've used exact 52-week periods instead of calendar years, which means that the periods covered regress slightly into late February by the end. Since I'm only after a reasonably accurate ballpark figure, I've simply eyeballed the excess mortality gap from the charts (given below) produced by my method. For the underlying data, visit this Statistics Canada website. It has also been necessary to estimate the number of Covid deaths in the four age brackets used by Statistics Canada for excess death calculations (0-44; 45-64; 65-84; 85+) from the 10-year brackets used by the Public Health Agency of Canada (in their March 6, 2023 Covid epidemiology update; see below). My rule of thumb, given the extreme age gradient for Covid deaths, is that for any given 10-year category, two thirds of the deaths will be in the top half and one third in the bottom. In the case of the 80+ category, I again assumed that 80-84 represents about a third of the entire category, even though it goes beyond 89: while there is a wider age range, there are going to be far fewer people that survive into the older range. I've also rounded to the nearest 100 for the sake of simplicity.
Without further ado, here are the excess mortality charts. In contrast to my earlier graphs, each point represents the preceding year (e.g. the point above 2021 on each graph covers the period from March of 2020 to March of 2021):
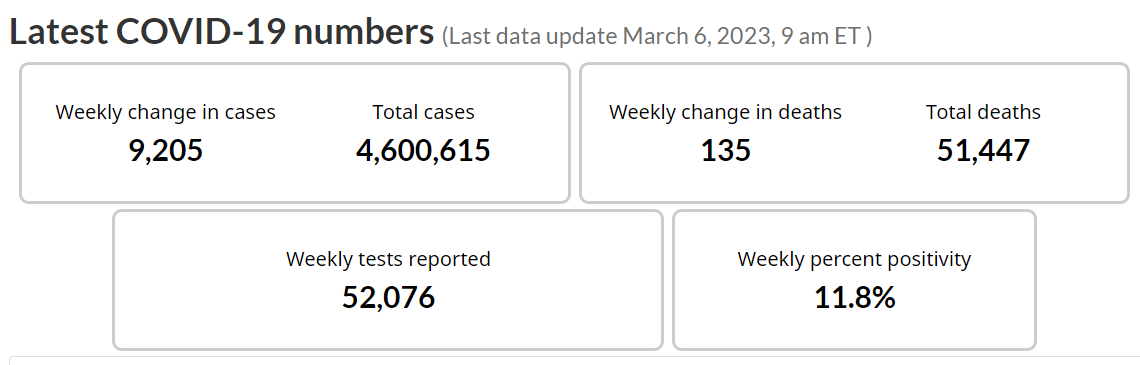
According to PHAC, as of March 6, 2023, there were 51447 Covid deaths:
For some reason, the total number of deaths (“n=36213”) is significantly lower in Figure 4:
I’m going to assume that there is a reasonable explanation for this, and take the higher figure as the official one.
Based on the above, and using the assumptions I mentioned earlier, 'Covid deaths' as of March 6, 2023 are approximately as follows:
0-44: 1200
45-64: 7800
65-84: 24600
85+: 20700
We can then calculate the number of excess deaths that were not said to be due to Covid (i.e. ‘non-Covid excess mortality’):
0-44: 9000 - 1200 = 7800
45-64: 9500 - 7800 = 1700
65-84: 42400 - 24600 = 17800
85+: 9000 - 20700 = -11700
A number of observations about this three-year period can be made from the data given above:
The total number of non-Covid excess deaths across the bottom three age categories (27300) is almost as high as the Covid deaths in that same range (29600). Whatever it was that Public Health wanted us to do to keep people safe, it doesn’t seem to have worked very well. No matter how anyone tries to cut it, sacrificing that many people in order to attempt to control a virus makes no sense at all, epidemiologically or ethically. Such control, needless to say, only existed in the fertile imaginations of those who embraced the ‘War on Covid’.
Almost 8000 younger people (0-44) across the country died (beyond what was expected) while we were fighting Covid, a condition that virtually none of them had any reason to be worried about. I would also be willing to bet that most of the 1200 or so ‘Covid deaths’ in this age range were incidental, and that the health of these individuals was heavily compromised by other conditions.
As with the Ontario data (and this almost certainly shows up everywhere), the negative non-Covid excess mortality means that a large percentage (more than half) of the 85+ deaths that were labelled as ‘Covid related’ would have happened anyway. Nor is it at all clear that every death with the Covid label in the 65-84 range represents additional mortality beyond what would have been expected.
Both for the youngest cohort who have the most to lose (0-44) and for the largest cohort of especially vulnerable people (65-84), excess mortality got progressively worse over the three-year period. For the other two age ranges mortality remained at an elevated level even in the third year. Again, whatever it thought it was doing, Public Health really seems to have dropped the ball, to say the least. The health of the public experienced a sharp decline under its guidance.
Can we be more specific about how, exactly, the many additional non-Covid excess deaths came about? Were there any noticeable shifts in the official causes of death recorded by Statistics Canada for this three-year period? To address these questions we may turn to another Statistics Canada website, “Deaths and age-specific mortality rates, by selected grouped causes”. The fit isn’t perfect, since StatsCan uses calendar years while I’ve focussed on ‘Covid-response years’, i.e. March to March. But for a big picture analysis, it is more than enough. From the website just given, data can be downloaded as far back as 2000, which provides ample context for any deviation in trends. Looking over this data, a few things are worthy of note.
First of all, neither of the ‘big two’ causes of death (cancer and cardiovascular disease) show any obvious deviation from trends. It will be interesting to see where the 2023 numbers end up. Nor does the third leading cause of death, accidents, end up noticeably outside of its expected levels in the Covid-response era. Leaving aside respiratory disease for the moment, there are two causes of death whose levels stand out as abnormal across 2020, 2021, and 2022: Alzheimer’s (lower than expected) and chronic liver disease and cirrhosis (higher than expected):
The Alzheimer’s data do not yield a high-fit trendline, but unless one wishes to argue that the dramatic downturn in 2018 and 2019 got even more dramatic after 2019 instead of some kind of upward correction, it is clear that the Covid-response era generated significantly fewer Alzheimer’s deaths than expected, at least on paper. Even with a more horizontal trendline (from, say, 2008) there would still be a deficit of a few thousand deaths. One may legitimately wonder: were these (elderly) individuals assigned to the ‘Covid death’ category? It is hard to see how Covid interventions would have, on their own, lessened the impact of Alzheimer’s; if anything, the reverse should be the case. Elder neglect was rampant.
The higher-than-normal incidence of liver disease and cirrhosis stands out quite clearly from a rock-solid trendline, perhaps partly related to higher levels of alcohol consumption during lockdowns.
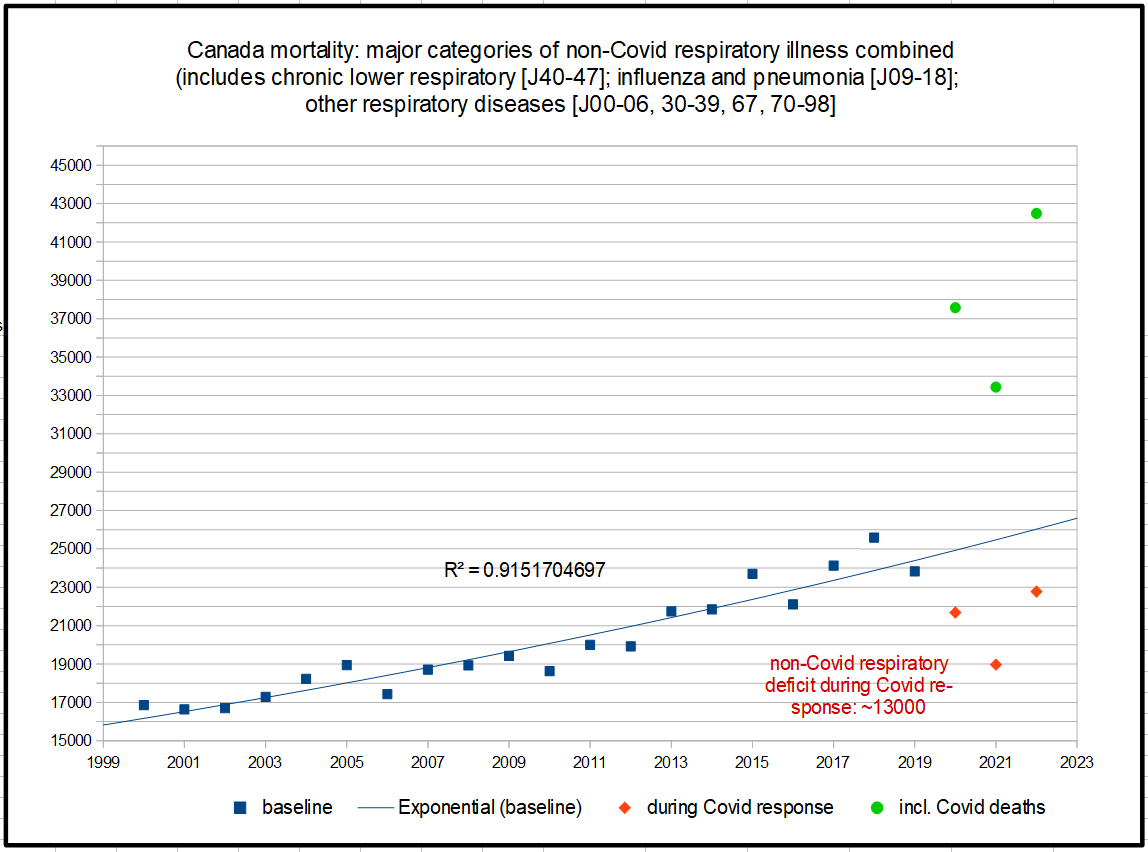
When it comes to respiratory illness, the picture is complicated by the new category of ‘Covid’, which is dominated by respiratory symptoms, even if it also involves other systems in the body. I wondered: what happens to non-Covid (i.e. traditional) respiratory illness, across all categories combined, during the Covid-response era?
The trendline fit here is pretty solid (exponential rather than linear in this case). As we can see, there is a sharp drop in traditional respiratory causes of death beginning in 2020. The green circles represent the total respiratory deaths with Covid added in. What are we to make of this? The Covid Myth propagated by Public Health would have us believe that interventions brought levels of traditional respiratory illness mortality significantly down. But at the same time, at least when considered as a respiratory disease, Covid-19 seems not to have been mitigated at all. It is at this point, of course, that Public Health rolls out the ‘it would have been much worse’ argument: ‘True, our interventions did not stop the virus in its tracks, but they did manage to avert an even greater catastrophe!’ As many by now have pointed out, this conviction has no grounding in empirical evidence but is spun out of made-for-purpose models that provide convenient (and non-falsifiable) after-the-fact justifications for the reckless policies that were implemented in the name of ‘science’. It seems far more likely that most of the 13000 or so respiratory deaths that went missing in 2020-2022 represent people who would have died anyway and were labelled as ‘Covid deaths’. At least this is a reasonable position to hold; I remain open to alternative explanations. Respiratory disease is inherently difficult to mitigate, and the vulnerable portion of the population didn’t magically disappear when Covid-response interventions began.
There is one remaining feature of the ‘causes of death’ data worthy of mention. In fact, it is the most obvious deviation from trend, and should make anyone wonder how such a shift could take place so quickly. I’m referring to the ‘fudge’ category of “Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified”:
There’s no point in trying to add a trendline here; the problem is obvious. How can there suddenly be so many unclassified deaths? Is this just a lag in the data? Will all these deaths show up in other categories in future publications? I have no idea. What’s clear is that, apart from blaming it all on Covid and refusing to acknowledge that lockdowns and other interventions may have played a role, the Public Health Agency of Canada really has little idea of why excess mortality has gotten so high in recent years. Or at least, if they do, they’re not willing to tell us.